Peroneal Tendinopathy – Symptoms, Causes, and Treatment Options
Peroneal tendinopathy is a painful condition affecting the tendons that run along the outside of your ankle and foot. It often causes pain, swelling, and stiffness on the outer ankle, especially during walking, running, or standing for long periods. This condition is common in athletes, active adults, and anyone with repetitive ankle strain.
Many people with peroneal tendinopathy find relief and faster recovery through CARESPACE services. Physiotherapy for peroneal tendinopathy helps reduce pain, restore ankle stability, and strengthen the supporting muscles to prevent re-injury. Chiropractic care for peroneal tendinopathy can improve alignment, decrease stress on the ankle joint, and promote proper healing, while massage therapy for peroneal tendinopathy relieves muscle tightness, improves circulation, and eases discomfort in the surrounding tissues. Together, these services provide a comprehensive approach to reducing pain and supporting long-term ankle health.
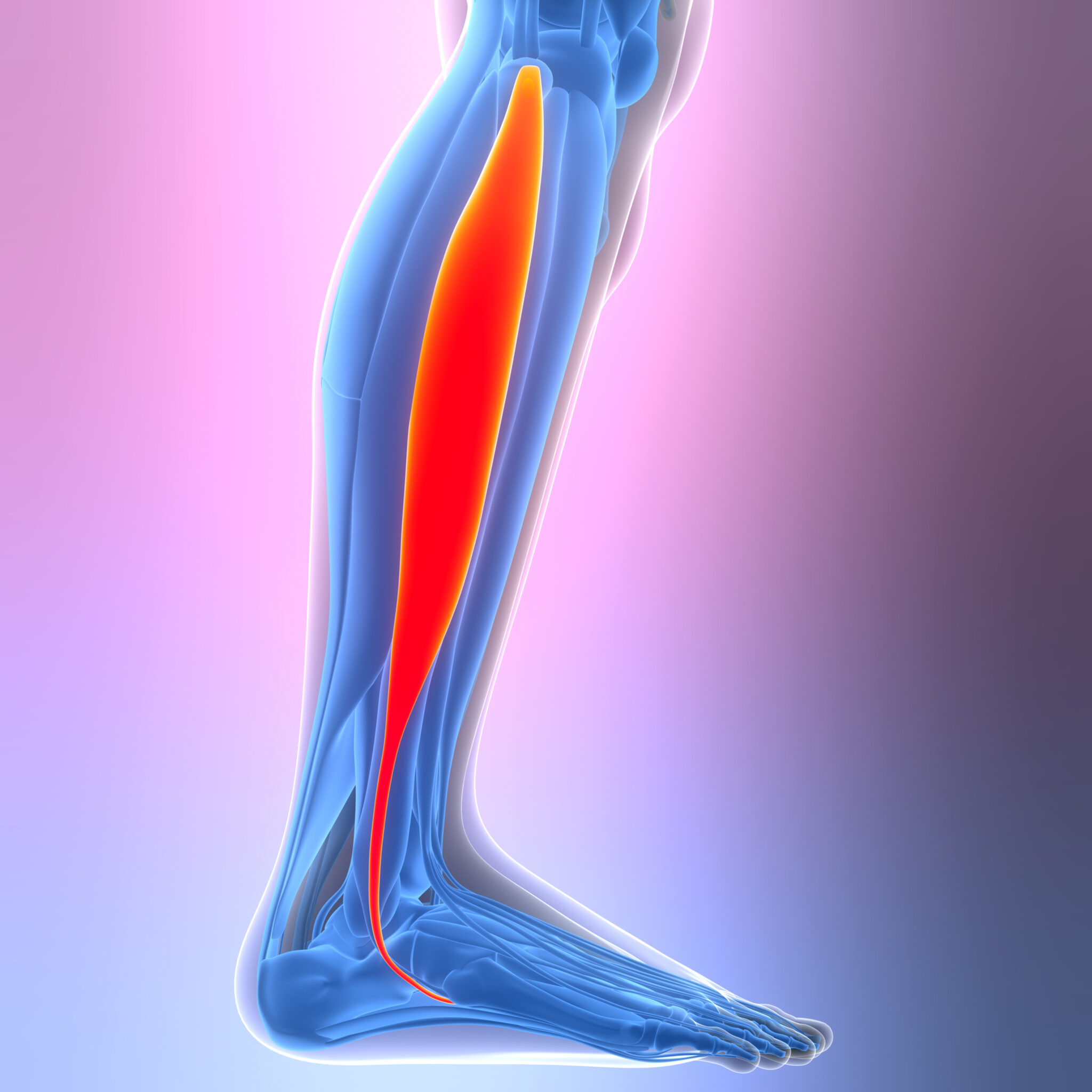
Overview of Peroneal Tendinopathy
Peroneal tendinopathy is an overuse injury of the peroneal tendons, which run behind the bony bump on the outside of your ankle (the lateral malleolus). These tendons stabilize your ankle and foot, especially when you push off, balance, or walk on uneven surfaces. When they become irritated or overloaded, tiny tears can develop, leading to inflammation, thickening, and pain.
How common is peroneal tendinopathy?
Although less common than Achilles tendon problems, peroneal tendinopathy is not rare. It is frequently seen in runners, dancers, and athletes in sports requiring sudden direction changes, such as soccer or basketball. According to studies, peroneal tendon injuries may be present in up to 35% of people with chronic ankle instability (van Dijk et al., 2010, British Journal of Sports Medicine, DOI: 10.1136/bjsm.2009.068163).
Daily life impact
Peroneal tendinopathy can affect everyday life in several ways:
- Work: Standing jobs like teaching, retail, or construction may worsen ankle pain.
- Sport: Running, jumping, or pivoting sports become difficult, sometimes forcing athletes to stop or modify training.
- Sleep: Night pain or discomfort when rolling onto the outside of the ankle can disturb rest.
- Relationships & mental health: Living with persistent pain can lead to frustration, reduced social activity, and anxiety about reinjury.
By understanding the condition and its risk factors, you can take steps toward effective treatment and prevention.
Symptoms of Peroneal Tendinopathy
The hallmark symptom of peroneal tendinopathy is pain and tenderness on the outer ankle, just behind the bony prominence. The discomfort often worsens with activity and improves with rest, but may progress if ignored.
What are the main symptoms of peroneal tendinopathy?
- Pain: Aching, sharp, or burning pain along the outer ankle or side of the foot.
- Swelling: Puffiness or thickening near the tendons.
- Stiffness: Worse in the morning or after prolonged sitting.
- Weakness or instability: Some people describe the ankle as “giving way.”
- Clicking or snapping: In severe cases, tendons may slip out of place, causing a popping sensation.
Severity spectrum
- Mild cases: Pain only after long activity.
- Moderate cases: Pain during normal walking, climbing stairs, or standing.
- Severe cases: Constant pain, instability, and sometimes tendon tears requiring surgical evaluation.
Functional impact
- Work: Difficulty standing or walking for long hours may reduce productivity.
- Sports: Athletes often cannot sprint, pivot, or land comfortably.
- Sleep: Pain when the foot rests sideways on a mattress can disturb sleep.
- Mood: Ongoing discomfort can contribute to stress, irritability, or even low mood.
Red flag signs
Seek medical attention if you experience:
- Sudden severe ankle pain after trauma (possible tendon rupture).
- Rapid swelling and bruising.
- Loss of ankle function or inability to bear weight.
These may indicate a tear, fracture, or severe instability requiring urgent care.
Causes and Risk Factors for Peroneal Tendinopathy
Peroneal tendinopathy is usually caused by repetitive stress or sudden overload of the tendons. The condition often develops over time but may also result from a sudden ankle sprain.
Common biomechanical causes
- Overuse: Repetitive running, jumping, or long-distance walking.
- Ankle instability: Prior ankle sprains that weakened support structures.
- Foot posture: High arches (supination) increase strain on the peroneal tendons.
- Improper footwear: Worn-out shoes or inadequate support.
- Muscle imbalances: Weakness in calf, hip, or core muscles altering gait.
Lifestyle and demographic risk factors
- Age: Middle-aged adults are more prone due to natural tendon degeneration.
- Occupation: Jobs requiring long hours of standing or walking increase strain.
- Sports participation: Activities like soccer, basketball, running, and ballet carry higher risk.
- Obesity: Excess body weight places more stress on tendons.
- Pregnancy: Hormonal changes and weight gain may alter ankle stability.
How is peroneal tendinopathy different from similar conditions?
- Achilles tendinopathy: Pain is located at the back of the ankle rather than the side.
- Ankle sprain: Usually involves sudden trauma with immediate swelling and bruising, while peroneal tendinopathy develops gradually.
- Plantar fasciitis: Causes heel and sole pain, not outer ankle discomfort.
Understanding these differences helps guide accurate diagnosis and treatment.
Diagnosis, Recovery, and Management of Peroneal Tendinopathy
Peroneal tendinopathy is most effectively addressed when properly diagnosed and managed with evidence-based strategies. This section explains how clinicians test for the condition, what recovery looks like at different severities, and how you can actively manage symptoms for long-term relief and prevention.
Diagnosis of Peroneal Tendinopathy
Peroneal tendinopathy is diagnosed through a combination of medical history, physical examination, and sometimes imaging. The goal is to rule out other causes of ankle pain and pinpoint tendon overload or degeneration.
How do doctors test for peroneal tendinopathy?
Your healthcare provider usually begins by asking about your symptoms, including when pain occurs (e.g., during activity, rest, or sleep). A physical exam follows, focusing on:
- Palpation: pressing along the outside of the ankle to check for tenderness.
- Movement tests: asking you to resist foot eversion (pushing your foot outward) while the clinician applies pressure. Pain during this test often indicates peroneal tendon involvement.
- Functional assessment: observing walking, running, or balancing on one leg to assess ankle stability.
When is imaging needed?
Imaging is not always required but may be used if symptoms are severe, unclear, or persistent:
- Ultrasound: dynamic imaging that can show tendon thickening, fluid buildup, or tendon slipping.
- MRI: detailed scan used to detect partial or full tears, chronic degeneration, or associated ankle conditions.
- X-rays: primarily used to rule out fractures or arthritis, not tendon damage itself.
Identifying the root cause
A complete diagnosis includes understanding what caused the tendon overload. This may involve:
- Gait analysis (to spot foot posture issues such as high arches).
- Review of footwear and sports training loads.
- Assessing for prior ankle sprains or instability.
Comparison note: Unlike an ankle sprain, which has a sudden onset with bruising and swelling, peroneal tendinopathy typically develops gradually from overuse.
Recovery Timeline and Prognosis for Peroneal Tendinopathy
Recovery depends on how severe the tendon injury is. Mild cases may resolve within weeks, while severe cases may take months and sometimes require surgical evaluation.
How long does peroneal tendinopathy take to heal?
- Mild cases: 4–6 weeks with rest, activity modification, and targeted rehab.
- Moderate cases: 2–3 months of structured therapy and load management.
- Severe cases: 6 months or longer, especially if tendon tears or chronic instability are present.
Factors affecting recovery
- Early treatment usually leads to faster outcomes.
- Recurrent ankle sprains or high arches may prolong recovery.
- Age and activity level: older adults or competitive athletes may heal more slowly.
Risk of recurrence
Recurrence is possible if the underlying biomechanical or lifestyle factors are not addressed. For example, returning to high-impact sport too quickly or continuing with unsupported footwear increases the risk of relapse.
Return-to-work and return-to-sport considerations
- Work: Desk workers may return quickly with modifications, while physically demanding jobs may require a longer phased return.
- Sport: A gradual return-to-sport plan usually involves strengthening, balance drills, and sport-specific training before full play.
- Lifestyle: Long-term management often includes ongoing ankle strengthening, supportive footwear, and weight management.
Decision pathway example:
- If symptoms are mild: Rest, supportive footwear, and guided exercises may be enough.
- If symptoms are moderate: Structured rehab with physiotherapy and bracing may be recommended.
- If symptoms are severe or nonresponsive: Surgical repair or advanced interventions may be considered.
Management of Peroneal Tendinopathy
Peroneal tendinopathy can often be managed successfully with a combination of rest, rehabilitation, and lifestyle changes. The key goals are pain reduction, tendon healing, and prevention of recurrence.
What’s the best way to manage peroneal tendinopathy at home?
Self-care strategies can help reduce pain and promote healing:
- Rest and activity modification – avoid high-impact activities that aggravate pain.
- Ice therapy – apply ice packs for 15–20 minutes after activity.
- Supportive footwear or ankle bracing – reduce tendon stress during daily activities.
- Strengthening exercises – focus on calf raises, resistance band eversion, and balance drills.
- Flexibility work – gentle stretching of calves and ankles to improve range of motion.
Step-by-step self-help & relief tips
- Rest and elevate your ankle when pain flares.
- Apply ice packs to reduce inflammation.
- Use supportive shoes with lateral stability.
- Begin gentle resistance band exercises when pain improves.
- Progress to balance training and sport-specific drills before full activity.
Therapy and professional support
- Physiotherapy: Strength, balance, and flexibility programs.
- Massage therapy: Helps reduce tension in surrounding muscles.
- Orthotics: Custom inserts may correct foot posture.
- Cognitive-behavioral strategies: Managing stress and pain-related anxiety improves outcomes.
- Lifestyle optimization: Weight management, nutrition, and structured exercise programs support tendon health.
Prevention strategies
- Gradually increase training loads.
- Replace worn-out footwear regularly.
- Cross-train with low-impact activities (e.g., cycling, swimming).
- Maintain ankle and hip strength to support balanced movement.
Multidisciplinary Coordinated Care for Peroneal Tendinopathy at CARESPACE
At CARESPACE, we take a team-based approach to peroneal tendinopathy, combining physical, mental, and lifestyle support so you can recover faster and reduce your risk of recurrence. Instead of treating only the symptoms, our coordinated care model addresses the root causes of tendon overload while supporting your whole health.
How does CARESPACE treat peroneal tendinopathy differently?
Most clinics focus on a single-discipline approach, such as physiotherapy alone. At CARESPACE, your care plan is built by a team. Physiotherapists, chiropractors, massage therapists, kinesiologists, and fitness trainers collaborate with dietitian, psychotherapists, and naturopathic doctors when needed. This means your treatment is not only about reducing pain, but also about restoring long-term ankle health, improving mobility, and addressing lifestyle and mental health impacts such as stress or insomnia.
For example, you may start with a physiotherapist to rebuild tendon strength, while also working with a massage therapist to ease calf tightness and a kinesiologist to improve balance and running form. If pain is causing sleep problems or anxiety, a psychotherapist or mental performance coach may also be involved.
Why does a team approach help peroneal tendinopathy recover faster?
Coordinated care helps reduce pain more quickly and prevents setbacks. When multiple providers share insights about your progress, they can adapt your plan seamlessly. This ensures you don’t waste time repeating tests or trying conflicting treatments.
Example of a team-based care pathway:
- Acute phase: Your physiotherapist prescribes rest, gentle mobility, and bracing if needed. A chiropractor checks alignment and biomechanics.
- Subacute phase: Massage therapy helps relieve muscle tension, while kinesiology and fitness training focus on gradual strength building.
- Maintenance phase: Nutrition guidance supports tissue healing, while psychotherapy or coaching helps you cope with stress and maintain healthy activity habits.
Compared with a single-discipline approach, multidisciplinary care is more effective at reducing recurrence risk, improving daily function, and helping you safely return to sport or work.
How does CARESPACE support your mental health during recovery?
Living with peroneal tendinopathy can be frustrating, especially if it limits sports, work, or daily activities. Stress, worry about re-injury, and even poor sleep from pain can slow recovery. CARESPACE integrates psychotherapy, mental performance coaching, and mindfulness strategies to help you build resilience.
- Psychotherapy: Supports you in managing pain-related anxiety, frustration, or lifestyle changes.
- Coaching: Helps set realistic goals and keep motivation high through rehab.
- Nutrition and naturopathic care: Addresses inflammation and overall wellness.
- Exercise therapy: Keeps you active with safe alternatives, helping mood and confidence.
This whole-person care model not only helps your ankle recover but also supports your overall well-being.
CARESPACE’s unique advantage for peroneal tendinopathy
Our advantage lies in personalized, coordinated care. At CARESPACE, you don’t just see one provider—you have a team that communicates and adjusts your plan across disciplines. That means:
- Faster pain relief through combined physical and manual therapies.
- Lower recurrence risk by correcting biomechanics and strengthening weaknesses.
- Improved quality of life through sleep, stress, and lifestyle support.
- A clear progression from injury → recovery → long-term prevention.
This approach is especially powerful for peroneal tendinopathy, a condition often caused by biomechanical imbalances and aggravated by stress or lifestyle factors. By treating both the physical and mental dimensions, CARESPACE helps you return not just to activity, but to living at your best.
Looking for information on a different condition? Visit our full Conditions List.
Peroneal Tendinopathy FAQs
The quickest relief usually comes from rest, ice, and reducing the activity that caused irritation. Supportive footwear or bracing may also help. In some cases, anti-inflammatory strategies like gentle massage or topical treatments provide added comfort. Longer-term, structured rehabilitation and strengthening are needed to fully resolve the condition.
This content is for informational purposes only and is not a substitute for professional medical advice. If you think you may have peroneal tendinopathy, consult a qualified health provider.
Mild cases may improve with rest and self-care, but most require targeted strengthening and rehabilitation to prevent recurrence. Unlike a simple muscle strain, tendon issues often persist if the underlying cause, such as poor foot mechanics or overuse, is not corrected.
This content is for informational purposes only and is not a substitute for professional medical advice. If you think you may have peroneal tendinopathy, consult a qualified health provider.
If ankle pain persists for more than two weeks, worsens with activity, or interferes with daily tasks, it’s time to seek medical advice. You should also consult a professional immediately if you experience sudden swelling, bruising, or difficulty bearing weight, as these may indicate a more serious injury.
This content is for informational purposes only and is not a substitute for professional medical advice. If you think you may have peroneal tendinopathy, consult a qualified health provider.
The best exercises focus on strengthening the peroneal muscles and improving ankle stability. Examples include resisted ankle eversion, single-leg balance drills, and controlled calf raises. Stretching the calves and foam rolling may also reduce tension that aggravates the tendons. Always progress slowly and seek professional guidance to avoid overloading the tendon.
This content is for informational purposes only and is not a substitute for professional medical advice. If you think you may have peroneal tendinopathy, consult a qualified health provider.
Prolonged standing, especially on hard surfaces, can worsen symptoms because it keeps the tendons under constant load. Sitting generally provides relief, but if poor posture or unsupportive footwear are involved, pain may linger even at rest. Alternating positions and using supportive shoes can help minimize strain.
This content is for informational purposes only and is not a substitute for professional medical advice. If you think you may have peroneal tendinopathy, consult a qualified health provider.
No, surgery is rarely the first option. Most people recover with conservative treatments like physiotherapy, bracing, and strengthening programs. Surgery is typically reserved for severe or chronic cases that do not improve after months of non-surgical care.
This content is for informational purposes only and is not a substitute for professional medical advice. If you think you may have peroneal tendinopathy, consult a qualified health provider.
Prevention focuses on strength, flexibility, and good biomechanics. Regular ankle-strengthening exercises, supportive footwear, and gradual increases in training intensity reduce risk. Avoiding uneven surfaces and adding cross-training activities also help prevent overload.
This content is for informational purposes only and is not a substitute for professional medical advice. If you think you may have peroneal tendinopathy, consult a qualified health provider.
Both cause pain on the outer ankle, but the source is different. A sprain involves torn ligaments, often after a sudden twist, while tendinopathy results from gradual overuse or biomechanical stress on the peroneal tendons. Sprains may cause bruising and swelling immediately, while tendinopathy usually develops slowly over time.
This content is for informational purposes only and is not a substitute for professional medical advice. If you think you may have peroneal tendinopathy, consult a qualified health provider.
Articles on Peroneal Tendinopathy
For more information, you can view all peroneal tendinopathy articles on our resource hub.
Authorship & Disclaimer
Reviewed by: Aayush Mehta, Physiotherapist
Last Updated: October 20th, 2025
Disclaimer: This content is for informational purposes only and is not a substitute for professional medical advice. If you think you may have Peroneal Tendinopathy, consult a qualified health provider.
