Compression Fractures – Symptoms, Causes, and Treatment Options
A compression fracture is a type of spinal injury that happens when one or more bones in your spine (called vertebrae) collapse or break. This often leads to sudden back pain, height loss, and changes in posture such as a stooped or hunched back. Compression fractures can range from mild to severe and have a big impact on your ability to move, work, and enjoy daily activities.
Many people with compression fractures find relief and regain function with physiotherapy for compression fractures, where gentle exercises and treatments help restore mobility and build strength safely. Chiropractic care for compression fractures can support proper spinal alignment and reduce strain on surrounding areas. Massage for compression fractures may ease muscle tension and improve circulation, helping to manage pain and stiffness. Kinesiology for compression fractures provides guided movement strategies to rebuild stability, restore confidence, and prevent future issues. Together, these services offer a supportive path to healing and improved quality of life.
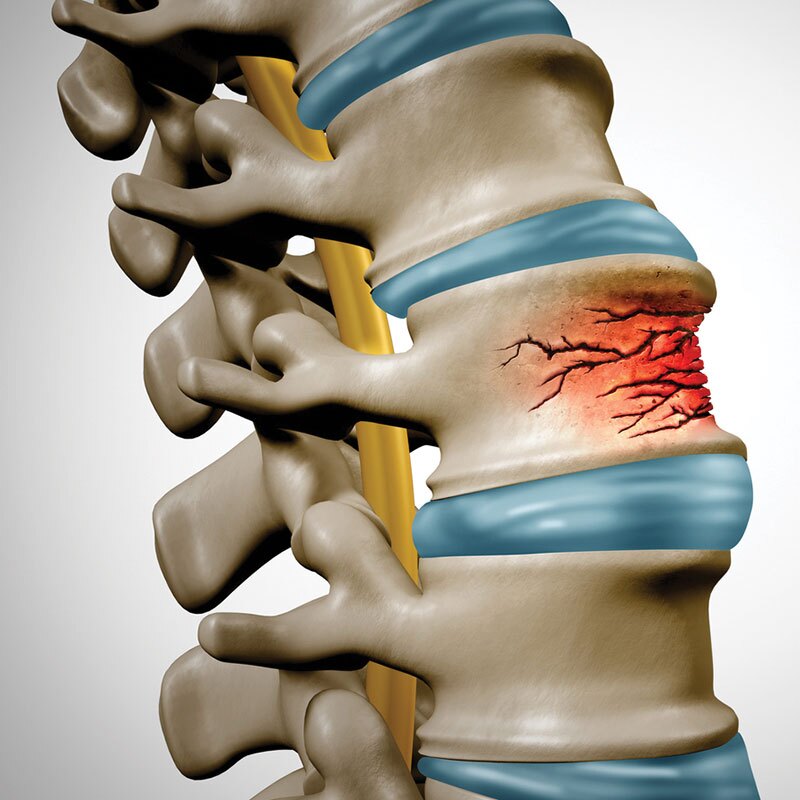
Overview of Compression Fractures
A compression fracture is when a vertebra in your spine weakens and collapses, usually in the mid to lower back. It can happen suddenly after an injury, or gradually over time due to conditions like osteoporosis (bone thinning).
How common are compression fractures?
Compression fractures are the most common type of spinal fracture. According to the International Osteoporosis Foundation, an estimated 1.4 million vertebral fractures occur worldwide every year, with prevalence increasing with age (Kanis et al., 2004, Osteoporosis International). Women are more at risk due to postmenopausal bone loss, but men also develop these fractures, especially later in life.
Why compression fractures matter
These fractures are more than just a broken bone—they can affect how you move and feel every day:
- Work & Productivity: Jobs that require lifting, standing, or sitting for long periods may become painful.
- Sport & Activity: Physical activity may be restricted, reducing fitness and independence.
- Sleep: Lying flat can be painful, leading to poor sleep quality.
- Relationships: Chronic pain may affect mood and the ability to enjoy time with loved ones.
- Mental Health: Ongoing discomfort, fear of movement, and changes in posture can lead to anxiety, frustration, or depression.
How are compression fractures different from other back injuries?
- Unlike muscle strains, compression fractures involve actual bone damage.
- Unlike herniated discs, which affect the cushioning tissue between vertebrae, compression fractures involve collapse of the bone itself.
- Unlike osteoporosis without fracture, compression fractures already represent structural damage.
Reference:
Kanis, J. A., Johnell, O., De Laet, C., Jonsson, B., Oden, A., & Ogelsby, A. K. (2004). International variations in hip fracture probabilities: Implications for risk assessment. Osteoporosis International, 13(7), 519–527. https://doi.org/10.1007/s00198-002-1344-2
Symptoms of Compression Fractures
The main symptom of a compression fracture is sudden, sharp back pain, often triggered by a minor fall, lifting, or even sneezing. Some fractures develop slowly, with pain that builds over time.
What are the main symptoms of compression fractures?
- Sudden, severe back pain after a minor injury or even normal activity.
- Pain that worsens with movement such as standing, bending, or lifting.
- Loss of height (sometimes several inches) as vertebrae collapse.
- Rounded or hunched posture (kyphosis) due to spinal changes.
- Stiffness and limited mobility in the back.
- Nerve symptoms such as tingling, numbness, or weakness if the fracture presses on spinal nerves.
How severe can compression fracture symptoms be?
- Mild fractures may cause only moderate pain and stiffness.
- Moderate fractures can make walking, sitting, or sleeping very uncomfortable.
- Severe fractures may lead to disability, nerve compression, or spinal deformity.
Red flag signs to watch for
See a doctor right away if you notice:
- Sudden back pain after a small fall or normal activity.
- Numbness, tingling, or weakness in your legs.
- Trouble controlling your bladder or bowels (could indicate spinal cord compression).
Daily life impact of compression fractures
- Work: Long hours at a desk or lifting can worsen pain.
- Sport: Activities like running or weightlifting may be limited.
- Sleep: Finding a comfortable position may be difficult.
- Mood & Mental Health: Ongoing pain can lead to frustration, irritability, or social withdrawal.
Reference:
Cummings, S. R., & Melton, L. J. (2002). Epidemiology and outcomes of osteoporotic fractures. The Lancet, 359(9319), 1761–1767. https://doi.org/10.1016/S0140-6736(02)08657-9
Causes and Risk Factors for Compression Fractures
Compression fractures are most often caused by weakened bones, trauma, or underlying disease. Osteoporosis is the leading cause, but lifestyle factors, posture, and occupation also play important roles.
What causes compression fractures?
- Osteoporosis: The most common cause, leading to weak and brittle bones that fracture easily.
- Trauma: Car accidents, falls, or sports injuries can compress spinal bones.
- Cancer: Tumors that spread to the spine can weaken vertebrae.
- Bone disease: Conditions like Paget’s disease may contribute.
Who is most at risk?
- Older adults, especially women after menopause.
- People with osteoporosis or low bone density.
- Those with a history of fractures.
- People in physically demanding jobs involving lifting or twisting.
- Individuals with poor posture or spinal degeneration.
- Patients on long-term corticosteroid use (which weakens bone).
Lifestyle factors that increase risk
- Age: Bone density declines naturally with aging.
- Obesity: Adds pressure on the spine and worsens posture.
- Smoking & alcohol: Both weaken bone health.
- Sedentary lifestyle: Lack of activity reduces bone strength.
- Diet: Low calcium or vitamin D intake increases risk.
- Pregnancy & postpartum: Hormonal changes may temporarily weaken bone.
How are compression fractures different from hip or wrist fractures?
While hip and wrist fractures also occur from osteoporosis, compression fractures may happen silently and only be discovered after height loss or back pain. This makes awareness and early detection critical.
Reference:
Rosen, H. N., Drezner, M. K., & Favus, M. J. (2021). Vertebral compression fractures: Clinical manifestations and management. UpToDate. Retrieved from https://www.uptodate.com/contents/vertebral-compression-fractures
Diagnosis, Recovery, and Management of Compression Fractures
Compression fractures of the spine can cause sudden pain, posture changes, and loss of mobility. Getting the right diagnosis, understanding recovery timelines, and following evidence-based management strategies are essential to healing and preventing future fractures. This section explains how compression fractures are diagnosed, what to expect in terms of recovery, and the most effective ways to manage the condition.
Diagnosis of Compression Fractures
Compression fractures are diagnosed through clinical evaluation, physical examination, and imaging tests. Because back pain has many possible causes—from muscle strain to herniated discs—healthcare providers carefully assess symptoms and use imaging to confirm the presence of a fracture.
How do doctors test for compression fractures?
Medical history and symptoms: Doctors will ask when your pain began, whether it followed an injury, and how it affects daily activities.
- Physical examination: This includes checking posture, range of motion, tenderness along the spine, and signs of nerve involvement such as numbness, tingling, or weakness.
- Imaging tests:
- X-rays show collapsed vertebrae and confirm the presence of a fracture.
- MRI scans identify new fractures, soft tissue damage, and whether spinal nerves are compressed.
- CT scans provide detailed images of the spine to rule out complex fractures.
- Bone density scans (DEXA) may be ordered if osteoporosis is suspected.
How is the root cause identified?
Doctors look beyond the fracture itself to determine why it happened. If a fracture occurred after minimal trauma (like bending or coughing), osteoporosis is often the underlying cause. If a younger person suffers a fracture from a significant accident, trauma is the likely driver. In some cases, cancer or other bone diseases are investigated.
How is a compression fracture different from other spinal conditions?
- Muscle strain: Pain improves with rest and does not cause vertebral collapse.
- Herniated disc: Causes radiating leg pain (sciatica) but not vertebral collapse.
- Spinal stenosis: Leads to gradual narrowing of the spinal canal and nerve compression, not sudden collapse.
Reference:
Rosen, H. N., Drezner, M. K., & Favus, M. J. (2021). Vertebral compression fractures: Clinical manifestations and management. UpToDate. Retrieved from https://www.uptodate.com/contents/vertebral-compression-fractures
Recovery & Prognosis for Compression Fractures
Recovery timelines for compression fractures vary depending on severity, age, bone health, and whether underlying conditions like osteoporosis are treated.
How long does it take to recover from a compression fracture?
- Mild cases: Pain may improve within 6–8 weeks with rest, bracing, and gentle rehabilitation.
- Moderate cases: Recovery often takes 3–6 months, with ongoing physical therapy to restore mobility.
- Severe cases: Multiple fractures or fractures with nerve involvement may take 6–12 months or longer, with some permanent effects.
If/Then Recovery Pathway
- If you have a single, mild fracture and good bone health, then you may recover within weeks using conservative care.
- If you have multiple fractures or osteoporosis, then recovery will likely require long-term management and lifestyle adjustments.
- If nerve compression or deformity occurs, then surgery or advanced interventions may be considered.
Return-to-work, sport, and lifestyle outcomes
- Work: Light desk work may resume in weeks, while heavy labor may require months of recovery.
- Sport: Low-impact activities like walking or swimming are encouraged during healing, but high-impact sports are delayed until bones are stronger.
- Lifestyle: Long-term bone health maintenance—through nutrition, exercise, and osteoporosis treatment—reduces the risk of future fractures.
- Long-term outlook
Some people recover fully, but others experience chronic back pain, height loss, or posture changes. Early diagnosis, bone-strengthening treatment, and rehabilitation improve long-term outcomes and reduce recurrence.
Reference:
Kado, D. M., Browner, W. S., Palermo, L., Nevitt, M. C., Genant, H. K., & Cummings, S. R. (1999). Vertebral fractures and mortality in older women: A prospective study. Archives of Internal Medicine, 159(11), 1215–1220. https://doi.org/10.1001/archinte.159.11.1215
Management of Compression Fractures
Management of compression fractures focuses on relieving pain, supporting healing, and preventing future fractures. This includes medical care, physical strategies, and long-term lifestyle adjustments.
What’s the best way to manage compression fractures at home?
- Posture: Maintain upright posture to reduce spinal stress.
- Ergonomics: Use supportive chairs and mattresses to protect the spine.
- Activity modification: Avoid heavy lifting, twisting, or high-impact movements during recovery.
- Pain management: Heat packs, over-the-counter medications, or prescribed pain relievers may help.
- Bone health: A diet rich in calcium and vitamin D supports healing.
Step-by-Step Self-Help & Relief Tips
- Gentle movement: Take short walks daily to maintain circulation and prevent stiffness.
- Posture reset: Every hour, check your sitting and standing position to avoid hunching.
- Back-friendly stretches: Light stretching of hamstrings and hip flexors reduces strain on the spine.
- Supportive bracing: If prescribed, wear a spinal brace to limit movement and aid healing.
- Sleep comfort: Use pillows under the knees (when on your back) or between knees (on your side) for spinal alignment.
Each of these steps reduces pain while supporting recovery and minimizing the risk of new fractures.
Professional care options
- Physical therapy: Improves strength, flexibility, and posture.
- Medication: May include pain relievers, bone-strengthening drugs (bisphosphonates), or hormone-related therapies for osteoporosis.
- Interventional care: In some cases, minimally invasive procedures like vertebroplasty or kyphoplasty stabilize the fractured bone.
- Lifestyle programs: Exercise, nutrition counseling, and smoking cessation support bone health.
- Community and mental health support
Compression fractures can affect confidence, independence, and mental health. Joining support groups, working with counselors, or connecting with fitness communities can help maintain motivation and resilience during recovery.
Multidisciplinary Coordinated Care for Compression Fractures at CARESPACE
At CARESPACE, compression fractures are managed with a team-based, multidisciplinary approach that addresses not only the fracture itself but also your mobility, strength, posture, and mental well-being. Instead of relying on a single-discipline model, CARESPACE coordinates multiple professionals—from physiotherapists and chiropractors to psychotherapists and nutrition experts—working together to create a personalized recovery plan that supports both your short-term healing and long-term spinal health.
How does CARESPACE treat compression fractures differently?
Most traditional care for compression fractures focuses on pain medication, rest, and sometimes surgery. While these steps can be important, they often leave gaps in recovery—such as rebuilding strength, restoring confidence in movement, and preventing future fractures. CARESPACE takes a different approach by integrating multiple disciplines into one coordinated care pathway.
- Physiotherapy and chiropractic care work together to restore spinal mobility, improve posture, and reduce stiffness.
- Massage therapy and acupuncture help relieve muscle tension, promote circulation, and ease pain from compensatory strain.
- Kinesiology and fitness training build strength safely, focusing on core stability and bone-supporting exercises.
- Psychotherapy and mental performance coaching address pain-related stress, sleep difficulties, and coping strategies.
- Nutrition and naturopathic medicine strengthen bone health with evidence-based dietary guidance and natural support for inflammation.
By combining these disciplines, CARESPACE ensures that every part of your healing process is covered—physical, emotional, and lifestyle.
Why does a team approach help compression fractures recover faster?
Compression fractures affect your entire life—not just your spine. Pain, stiffness, and height loss can reduce your mobility and confidence, while the stress of recovery can affect your sleep and mood. A single treatment approach may ease one area of discomfort, but it often misses the bigger picture.
Key benefits of CARESPACE’s coordinated model:
- Faster results: When physiotherapy restores function and psychotherapy helps manage anxiety, your body and mind recover in sync.
- Lower recurrence risk: Nutrition, exercise, and posture training strengthen bone health and reduce chances of future fractures.
- Personalized care: Your plan is adapted based on your stage of healing, whether you are in acute recovery or long-term maintenance.
- Whole-person support: CARESPACE addresses not just pain but also sleep, mental health, and lifestyle.
What does a typical care journey for compression fractures look like at CARESPACE?
Your recovery plan at CARESPACE is built in phases, with each stage supported by a team of experts.
Acute Phase (first weeks after fracture)
- Physiotherapy assessment to identify safe movements and prevent stiffness.
- Massage therapy to ease tension in surrounding muscles compensating for spinal pain.
- Psychotherapy to manage stress and reduce fear of movement, which is common after a sudden fracture.
- Nutrition guidance to support bone repair with calcium, vitamin D, and protein.
Subacute Phase (1–3 months)
- Chiropractic adjustments and physiotherapy work to restore healthy spinal alignment and movement.
- Acupuncture may be used for pain relief and improved circulation.
- Kinesiology and exercise therapy begin low-impact strengthening, such as resistance band work and posture exercises.
- Mental performance coaching supports resilience, focus, and coping during longer recovery.
Maintenance Phase (long-term recovery and prevention)
- Fitness training builds endurance, core stability, and safe lifting mechanics.
- Massage therapy and acupuncture are used as needed to prevent flare-ups.
- Nutrition and naturopathic medicine focus on preventing osteoporosis and promoting overall bone health.
- Psychological care ensures better sleep, mood balance, and confidence in movement.
How is mental health integrated into compression fracture care at CARESPACE?
Pain doesn’t only affect your body—it affects your mind and emotions. At CARESPACE, mental health is built directly into recovery plans for compression fractures.
- Psychotherapy helps you cope with frustration, mood changes, and fear of re-injury.
- Sleep and stress management are addressed through counseling, mindfulness, and lifestyle coaching.
- Nutrition support helps regulate mood and reduce fatigue.
- Exercise and fitness training naturally improve mental health by releasing endorphins and rebuilding confidence in daily activity.
By addressing stress, insomnia, and coping challenges alongside physical recovery, CARESPACE helps you heal more completely.
Why CARESPACE’s multidisciplinary care offers an advantage over traditional treatment
Standard care often treats compression fractures in isolation—pain is managed with medication, and bone density may be addressed later. This fragmented approach leaves patients vulnerable to recurrence, poor posture, or chronic pain. CARESPACE’s multidisciplinary, evidence-based model ensures that all aspects of recovery are integrated into one cohesive plan.
The CARESPACE advantage:
- Seamless communication: Every provider on your team shares notes and progress updates.
- Personalized recovery plans: Care adapts as your condition improves, ensuring long-term results.
- Whole-body and whole-mind healing: Pain, posture, strength, nutrition, and emotional health are all addressed.
- Prevention focus: Rather than only reacting to fractures, CARESPACE builds resilience and bone strength to reduce future risks.
Putting it all together
At CARESPACE, you don’t just get treatment for your spine—you get comprehensive, team-based care that supports your body, mind, and lifestyle. From physiotherapy and chiropractic adjustments to psychotherapy, nutrition, and exercise training, your plan is designed to help you recover faster, move with confidence, and prevent future fractures.
This multidisciplinary coordinated model is what sets CARESPACE apart: instead of fragmented, single-discipline treatments, you receive a connected, evidence-based journey toward long-term health and resilience.
Related Conditions for Compression Fractures
Compression fractures often share symptoms with other spine and bone conditions, which can sometimes make diagnosis challenging. Understanding related and overlapping conditions helps you know when to ask for further evaluation.
- Osteoporosis: The leading cause of compression fractures, where bones become thin and brittle. Many people with osteoporosis have fractures without realizing it until they notice back pain or height loss.
- Spinal Stenosis: Narrowing of the spinal canal that causes leg pain and numbness, which may overlap with symptoms of compression fractures pressing on nerves.
- Herniated Disc: While this condition causes nerve pain and leg symptoms, it does not involve bone collapse.
- Arthritis of the Spine (Spondylosis): Chronic wear and tear can cause stiffness, pain, and posture changes that mimic fracture symptoms.
- Cancer-Related Fractures: Sometimes, tumors weaken spinal bones, leading to fractures that resemble those caused by osteoporosis.
Disclaimer: This content is for informational purposes only and is not a substitute for professional medical advice. If you think you may have compression fractures, consult a qualified health provider.
Looking for information on a different condition? Visit our full Conditions List.
FAQs About Compression Fractures
If you’re dealing with Compression Fractures, you may have questions about symptoms, causes, and the best treatment options available. Below, we’ve outlined the most important information to help you understand Compression Fractures, what recovery might look like, and how CARESPACE can support you with a personalized care plan.
The quickest relief usually comes from rest, bracing, and pain management strategies guided by a doctor. Over-the-counter pain relievers, ice or heat therapy, and supportive bracing can help reduce discomfort in the short term.
For longer-lasting relief, physiotherapy and posture training are essential. Unlike muscle strains, compression fractures require structured recovery, not just rest. Gentle movement helps prevent stiffness and maintains circulation, while medical treatments may include bone-strengthening medications or minimally invasive procedures like vertebroplasty.
This content is for informational purposes only and is not a substitute for professional medical advice. If you think you may have compression fractures, consult a qualified health provider.
Mild compression fractures can heal over time, especially with rest and conservative care. Many improve within 6–12 weeks, but healing depends on bone health, age, and lifestyle.
Without treatment, however, fractures can worsen, leading to posture changes, chronic pain, or additional fractures. Unlike a simple muscle sprain, compression fractures involve structural damage to bone, so professional guidance is important. Treating the root cause, such as osteoporosis, is key to preventing further fractures.
This content is for informational purposes only and is not a substitute for professional medical advice. If you think you may have compression fractures, consult a qualified health provider.
You should see a doctor right away if you experience sudden back pain after a minor fall or activity. Other warning signs include loss of height, hunched posture, or new numbness and tingling in your legs.
Unlike routine backaches, compression fractures signal structural weakness in the spine. Early evaluation helps confirm the diagnosis with imaging and ensures you get started on treatment to prevent long-term complications like spinal deformity. If your pain does not improve with rest or worsens quickly, medical care is essential.
This content is for informational purposes only and is not a substitute for professional medical advice. If you think you may have compression fractures, consult a qualified health provider.
Yes, prolonged sitting or standing can aggravate compression fracture symptoms. Staying in one position for too long may strain spinal bones and muscles.
Alternating between sitting, standing, and gentle movement reduces stiffness and pain. Unlike normal postural discomfort, compression fracture pain often feels sharper and worsens quickly with pressure. Supportive seating, ergonomic adjustments, and regular posture breaks help protect the spine during healing.
This content is for informational purposes only and is not a substitute for professional medical advice. If you think you may have compression fractures, consult a qualified health provider.
No, surgery is rarely the first choice for compression fractures. Most cases improve with conservative care such as medication, physical therapy, and bracing.
Surgery may be considered if pain is severe, the fracture is unstable, or there are neurological complications like numbness or weakness. Minimally invasive procedures such as vertebroplasty or kyphoplasty can help stabilize the bone. Unlike hip fractures, which often require surgical repair, compression fractures are often treated successfully without surgery.
This content is for informational purposes only and is not a substitute for professional medical advice. If you think you may have compression fractures, consult a qualified health provider.
Prevention focuses on strengthening bones and protecting your spine. This means treating osteoporosis, staying active with weight-bearing exercise, and maintaining good posture.
Lifestyle changes like quitting smoking, limiting alcohol, and eating a diet rich in calcium and vitamin D also protect bone health. Unlike isolated accidents, compression fractures often signal ongoing bone weakness, so long-term prevention is critical. With the right plan, many people reduce their risk of future fractures significantly.
This content is for informational purposes only and is not a substitute for professional medical advice. If you think you may have compression fractures, consult a qualified health provider.
Compression fractures are caused by collapsed vertebrae, while herniated discs involve soft tissue and arthritis involves joint wear and tear.
- Compression fractures: Sudden pain, height loss, and hunched posture.
- Herniated discs: Nerve pain radiating to legs (sciatica) but no bone collapse.
- Arthritis: Gradual stiffness and pain, but usually without sudden structural collapse.
These conditions can overlap, but imaging tests help clarify the diagnosis. Understanding these differences ensures you receive the most effective treatment.
This content is for informational purposes only and is not a substitute for professional medical advice. If you think you may have compression fractures, consult a qualified health provider.
Articles on Compression Fractures
For more information, you can view all compression fractures articles on our resource hub.
Authorship & Disclaimer
Reviewed by: Jessica Sealey, RMT
Last Updated: September 21st, 2025
Disclaimer: This content is for informational purposes only and is not a substitute for professional medical advice. If you think you may have a compression fractures, consult a qualified health provider.
